 
We conducted the search in MEDLINE, EMBASE, and CINAHL (untill 1 June 2017) without language restriction (see Appendix 1). The protocol was registered in PROSPERO (2015:CRD42015027687). The aim of the current review is to more specifically summarize and compare the evidence on the diagnostic accuracy of diagnostic imaging (CT, X-rays, myelography and MRI) identifying LDH in patients with low back pain and/or leg pain with surgery as a reference standard.Ī systematic review and meta-analysis, according to the guidelines of the Cochrane handbook of systematic reviews of diagnostic test accuracy studies. We have performed a large study evaluating the evidence om diagnostic accuracy of MRI and CT for all kinds of lumbar pathologies compared to various reference standards. In addition, discordance between patients’ clinical findings and MRI findings is also reported. However, the evidence for diagnostic accuracy of diagnostic imaging for LDH is still unclear. Plain radiography (X-ray) is the most commonly used technique due to its relative low cost and ready availability. 
metal implants or malalignment of the spine) myelography might replace MRI as the imaging modality of choice. Myelography involves injection of contrast medium in the lumbar spine, followed by X-ray, CT or MRI projections. Compared to MRI, CT is cheaper, the total testing time is shorter, and the availability of CT scanners is larger in hospital settings, but has the drawback of exposure to ionising radiation. 
CT is often used and available for detection of morphologic changes and has a well-recognized role in the diagnosis of herniated discs. 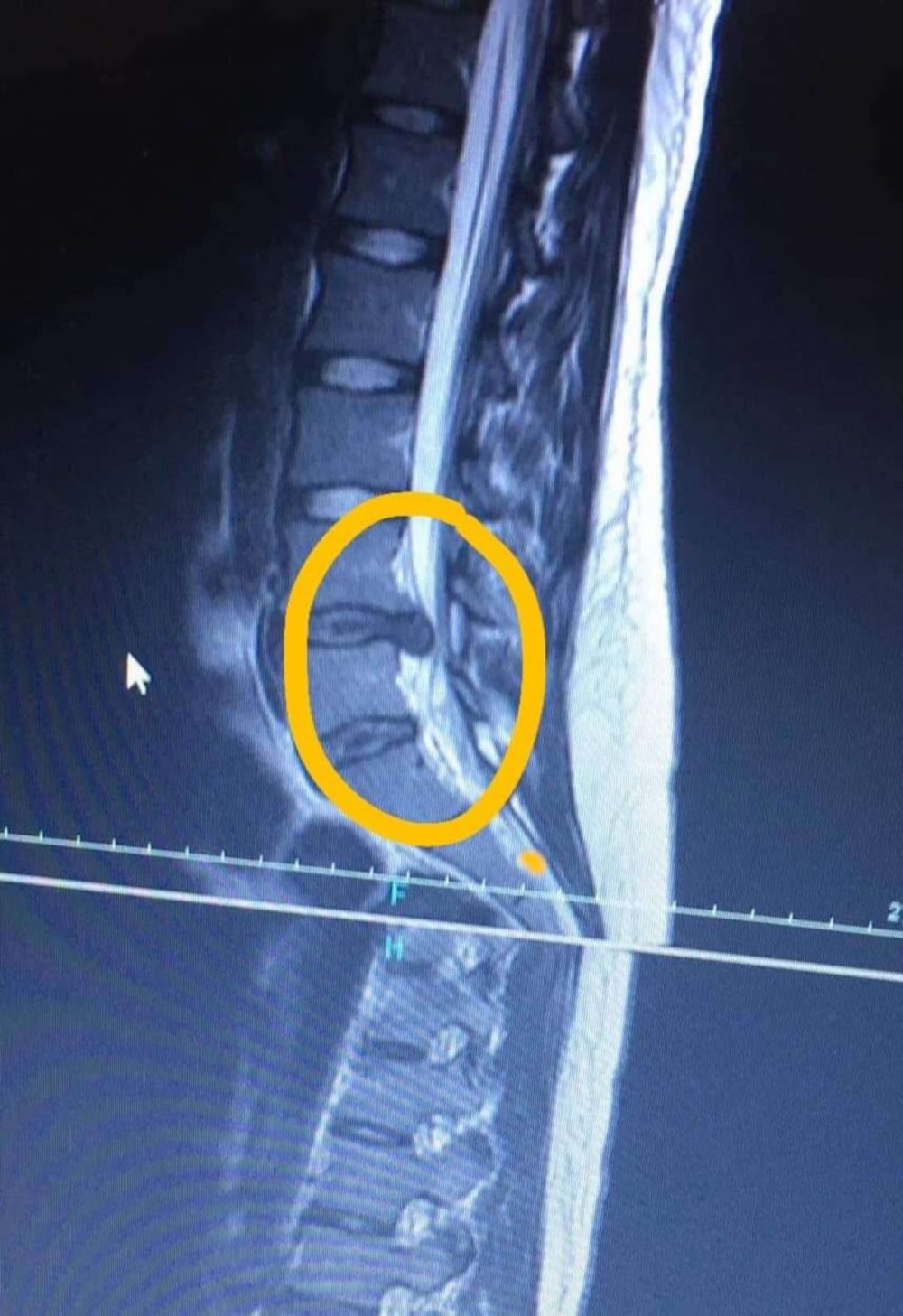
Currently MRI is the imaging modality of choice, as it has the advantage of not using ionising radiation and has good visualizing capacities especially of soft tissue. ĭiagnostic imaging can be done by Magnetic Resonance Imaging (MRI), Computed Tomography (CT), X-ray and myelography. Furthermore, diagnostic imaging can also be used to identify the affected disc level before surgery. Diagnostic imaging in patients with back pain and/or leg pain is often used to assess nerve root compression due to disc herniation or spinal stenosis and cauda equina syndrome. However, the diagnostic accuracy of both history taking and physical examination is still insufficient. Clinical guidelines recommend history taking and physical examination to rule out LDH diagnosis. LDH is the most common spine disorder requiring surgical intervention. Concerning the older techniques we found moderate diagnostic accuracy for all CT, myelography and MRI, indicating a large proportion of false positives and negatives.Īpproximately 5–15% of patients with low back pain suffer from lumbar disc herniation (LDH). The diagnostic accuracy of CT, myelography and MRI of today is unknown, as we found no studies evaluating today’s more advanced imaging techniques. The quality of evidence was moderate to very low. The summary estimates for MRI and myelography were comparable with CT (sensitivity: 81.3% (95%CI 72.3–87.7%) and specificity: 77.1% (95%CI 61.9–87.5%)). The prior probability of LDH varied from 48.6 to 98.7%. Nine studies investigated Computed Tomography (CT), eight myelography and six Magnetic Resonance Imaging (MRI). We found 14 studies, all but one done before 1995, including 940 patients. We calculated summary estimates of sensitivity and specificity using bivariate analysis, generated linked ROC plots in case of direct comparison of diagnostic imaging tests and assessed the quality of evidence using the GRADE-approach. Two review authors independently selected studies, extracted data and assessed risk of bias. We aim to summarize the available evidence on the diagnostic accuracy of imaging (index test) compared to surgery (reference test) for identifying lumbar disc herniation (LDH) in adult patients.įor this systematic review we searched MEDLINE, EMBASE and CINAHL (June 2017) for studies that assessed the diagnostic accuracy of imaging for LDH in adult patients with low back pain and surgery as the reference standard. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
